‘Malaria is simply a complex disease’
-
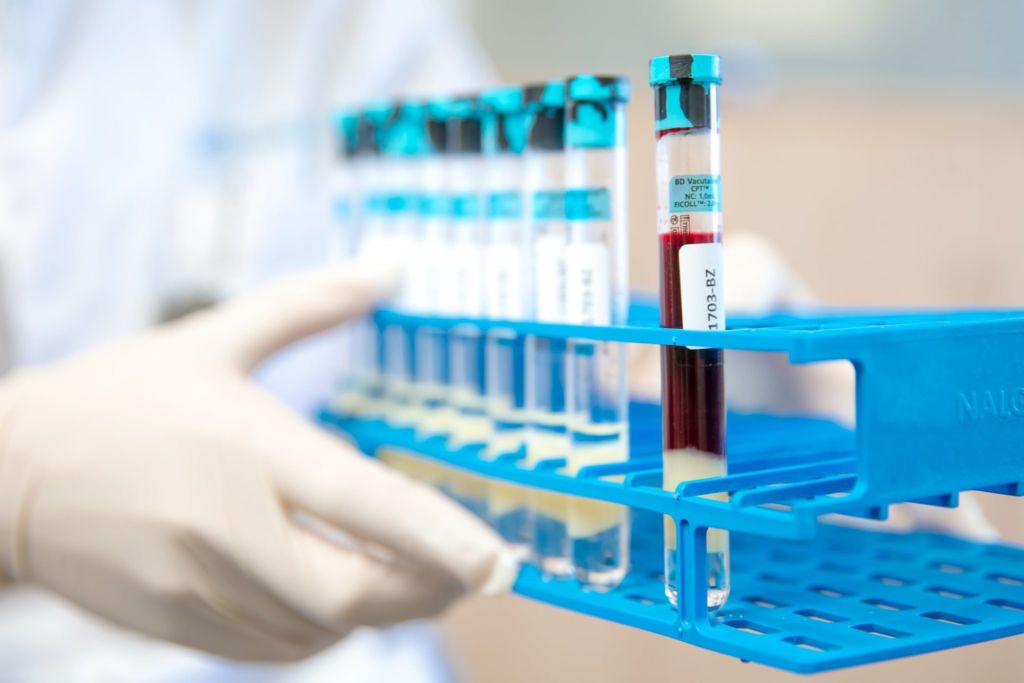
 Photo: Radboudumc.
Photo: Radboudumc.
Slowly but surely Nijmegen researchers are working on developing a malaria vaccine. ‘We should think more in terms of steps than breakthroughs,’ says Robert Sauerwein, Professor of Medical Parasitology and head of the Nijmegen Malaria Facility. Four questions about the progress of their research.
Ever since the 1960s researchers have been working on developing a vaccine against malaria. One of these research centres is located in Nijmegen and led by Professor of Medical Parasitology Robert Sauerwein. In the tropical rooms of the Malaria Facility, 10,000 mosquitoes are bred every week. To test the vaccines, some sixty test subjects per year volunteer to be injected with the malaria parasite.
So far, worldwide, only one vaccine has been approved by the European Medicines Agency (EMA), the institute that studies all the drugs that appear on the market. ‘This vaccine took over thirty years to develop, and was born of a collaboration between a large pharmaceutical company and the US Army,’ says Robert Sauerwein. ‘Unfortunately, it’s not a very good vaccine: it only protects 50% of the population, and not for very long.’
-
Why does it take so long to develop a vaccine?
Every year, malaria affects more than 200 million people and kills half a million, particularly in the tropics. Since the target group of malaria research is not located in the Western world – with the exception of Westerners who travel to the tropics – there’s not much funding for it. People in Africa have little money, so a vaccine can’t be expensive. This prevents companies from getting involved.
Add to this the fact that malaria is a complex disease. Mosquitoes carry the parasite, which in humans behaves differently depending on whether it appears in the blood or the liver, for example. ‘We don’t quite understand how the immune system responds to malaria,” says Sauerwein. “Fundamental research on this topic is as yet incomplete. This means vaccine research is often a question of trial and error.’
Thirdly, the directives for drug research are becoming more and more strict. The Nijmegen lab carries out research on humans, but also on mice, and most recently pigs. According to Sauerwein, these days it’s almost as difficult to experiment on animals as on humans. In both cases, the procedures are becoming ever more complicated, with sharp trade-offs between safety, costs and yield. The danger is a crippling bureaucracy, which slows down research progress.
-
What are the steps in malaria research?
In the first stage, malaria researchers try to identify a target for the vaccine: this could be a protein, a cluster of proteins, or even the entire parasite. In pre-clinical trials – in animals or in vitro (outside the body, Eds.) – researchers must demonstrate that their vaccine works as long as there’s enough immunity. In a model system in the lab, the vaccine must be shown to be effective and safe.
Once that’s the case, you make the transition to humans. In Phase 1 trials you have to show that the product is safe. Sauerwein: ‘You inject the vaccine in human subjects without them suffering any adverse effects – with the exception of an immune reaction which you can measure by taking a blood sample. By infecting test subjects with malaria you can show that the vaccine doesn’t only work in the lab, but also in real people.’
Ingi Veugen (21): ‘Blue blood vessels’
From September to November 2018, 21-year old Ingi Veugen, student in Cultural Anthropology and Development Studies, volunteered to take part in the malaria study. ‘An interesting excursion into the medical world,’ says Veugen.
During the first two weeks of the study Veugen had blood samples taken twice a day: in the morning before she went to class, and again in the evening. ‘Sometimes they would collect one vial, other times ten. At some point, my blood vessels were all blue’ (she laughs).
This was always followed by an interview with the doctor. ‘Among other things, I was asked to score how I felt on a scale of 1 to 5.’
At a later stage in the study, Veugen was required to allow a coffee cup full of mosquitoes have their way with the inside of her arm. ‘The first time, it was really scary. Luckily, there were four of us doing it at the same time. Afterwards, we were given a cream to take home to stop the itching.’
Veugen knew she might develop flu-like symptoms and a fever, but she suffered more from the effects of the drug than from the malaria itself. ‘I only had a temperature for one night; a friend of mine was in bed all week.’
Veugen sees the financial reward given to the study participants as a nice bonus. ‘To be honest, I probably wouldn’t have signed up without it.’
Once this works, the vaccine is tested in Africa, first on dozens of test subjects, and then, in Phase 2 in trials, on hundreds. ‘This is best done during the malaria season: how many cases of malaria occur in a group you vaccinated versus a group you didn’t vaccinate? Are there any significant differences?’
In Phase 3 trials the vaccine is tested on thousands of subjects in various countries and under different conditions. ‘These are large-scale, expensive studies, so you have to be sure your vaccine really works.’
If the vaccine survives this test, you contact the European Medicines Agency (EMA) and ask them to approve it. So far, worldwide, this has only happened once, but there are various projects in the pipeline.
- What role does Nijmegen have in malaria research?
The Nijmegen Malaria Facility, which employs around thirty researchers, is mostly known for its translational research: translating fundamental research to a product, bringing it to the field, and processing any findings in the vaccine. ‘We work from molecule to man to population,’ says Sauerwein. ‘These three elements feed one another. This allows us to take steps to speed up the development of new resources.’
At the moment, the three vaccines of the Nijmegen lab are all in the clinical trial phase. ‘In our lab we use highly controlled conditions to check whether our vaccines are effective and safe. We are now ready to move on to Phase 1 trials. TropIQ, a spin-off of the Novio Tech Campus hospital, has also developed a drug that’s entering the clinical trial phase. Whereas a vaccine prevents infection, this drug cures people who are already infected with malaria. We hope to be able to test the vaccines and the drug in Africa soon.’
- Will Nijmegen researchers ever develop a vaccine against malaria?
‘Of course we can dream,’ says Sauerwein, ‘but there’s no such thing as the perfect vaccine – at best you can have a good vaccine. The media are always asking whether we’ve finally made a breakthrough, but a vaccine is developed in small steps. There’s a dot on the horizon, though, that you have to keep moving towards. And once we have a vaccine, we’ll have new problems to solve, such as increasing resistance. There’s no one size fits all forever solution.’
Bram Slurink (19): ‘I now understand better how malaria works’
In the same round, Medical student Bram Slurink (19) also allowed himself to be bitten by malaria mosquitoes.
‘I saw on Facebook that they were looking for test subjects,’ says Slurink. ‘I think it’s important that there are enough test subjects for this kind of research, so I signed up. And as a student, it’s an easy way to make some money.’
Slurink didn’t suffer much from the mosquito bites. ‘They just itched a little. After being infected with malaria, I was slightly ill for two days, but not so that I had to stay in bed. I got heart palpitations when walking up the stairs and I was very tired. I didn’t really have a fever.’
Slurink enjoyed the contact with the doctors. ‘I talked to them about the study. I now have a better understanding of how malaria works.’
According to Slurink, a lot of people think the financial reward is based on the risks involved. ‘But that’s not the case: it’s about the time you devote to the study. Since I live close to the hospital, I didn’t get that much money.’
Nevertheless, a lot of people advised Slurink not to take part in the study. ‘And that while these kinds of studies are completely risk-free. The worst thing that could have happened was me lying in bed sick for a few days. It’s a risk I was prepared to take.’



